Advancing Comprehensive Integrative Pain Management
What Matters
to You?
AACIPM’s 2022 Highlights
AACIPM connects multi-stakeholders with a shared interest in modifying policy and payment design to improve access to whole person pain care.
Click on a topic to learn more.
PATIENT-CENTERED
Access to Care
and
Payment Design

CIPM Toolbox
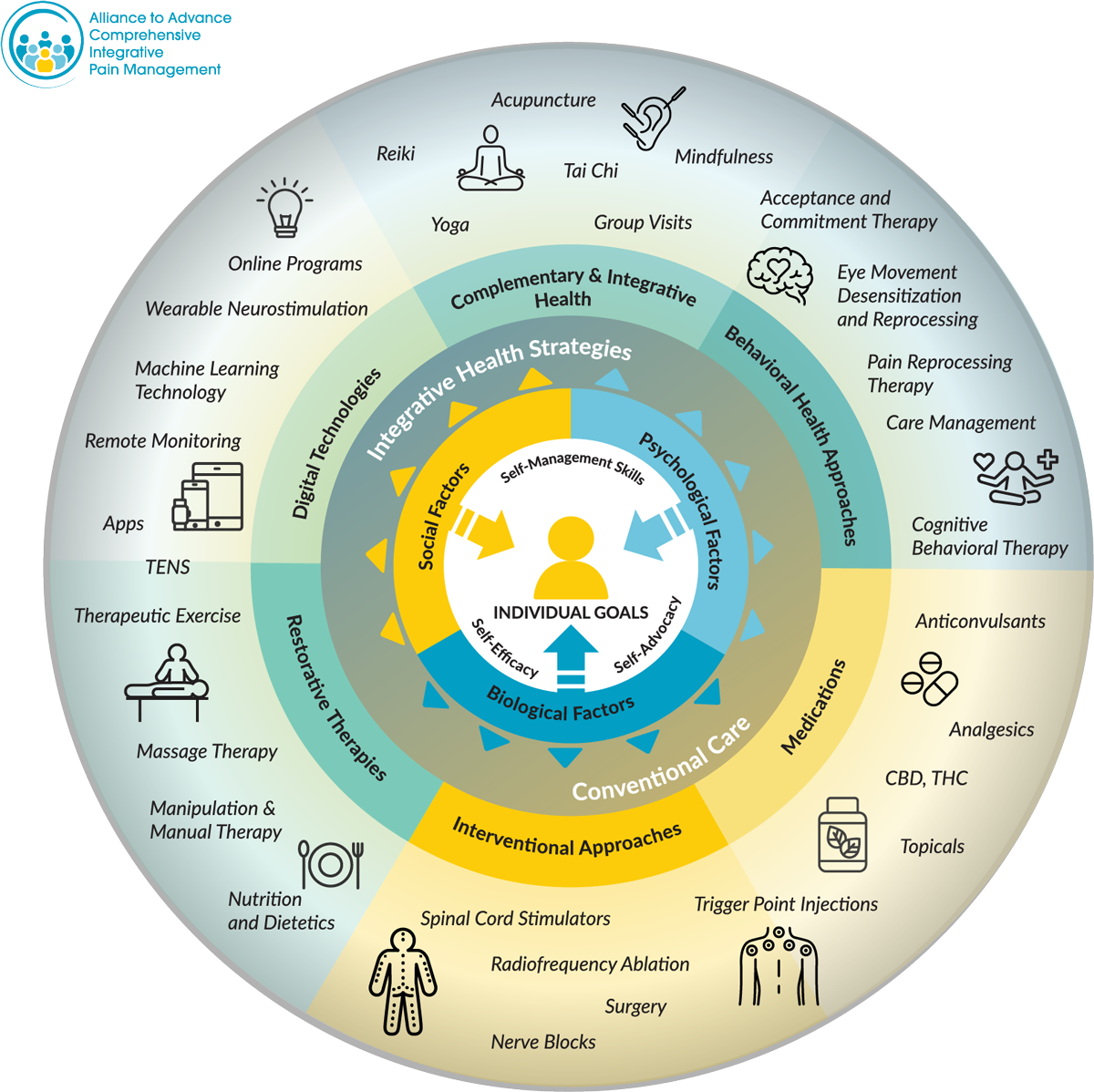
Comprehensive Integrative Pain Management (CIPM)
Citation: Comprehensive Integrative Pain Management Toolbox. Alliance to Advance Comprehensive Integrative Pain Management. August 2022. https://painmanagementalliance.org/what-is-cipm/
AACIPM offers this visual tool to illustrate and increase awareness of the various therapies that may be a part of whole person, multidisciplinary, multi-modal, evidence-informed, integrative pain management.
This does not represent an exhaustive list of interventions, and not all interventions will be covered, covered without limits and/or without patient out-of-pocket cost.”
Most services must be provided by a licensed or credentialed health care provider or community-based service provider.
AACIPM Releases Brief on Pediatric Pain
 Connecting the Dots to Advance Access to Comprehensive Integrative Pain Management (CIPM)
Connecting the Dots to Advance Access to Comprehensive Integrative Pain Management (CIPM)
Pediatric Pain: Promoting Access to Whole Person, Multimodal Pain Management for Children and Adolescents
Evidence-Based Tools for Providers, Care Options for Patients and Families, and Evidentiary Support for Policymakers
Our Youth are Hurting:
Reconsidering How We Treat and Prevent Children Living with Pain
Children are living through extraordinarily difficult times. For over two years, the COVID-19 pandemic has resulted in countless families facing financial insecurity, food scarcity, a highly dangerous contagion, the tragic and premature deaths of loved ones, and the emerging fallout of long-COVID. Rates of severe depression and suicide in our nation’s youth have skyrocketed, spurring leading pediatric groups to declare a national emergency in children’s mental health.1,2
A Paradigm Shift: Partnering & Aligning to Change Policy & Practice
AACIPM is a leader thoughtfully connecting key stakeholders and influencers towards the paradigm shift we all want to see – person-centered, evidence-based, comprehensive, integrative, integrated, interdisciplinary pain management.
NATIONAL AND STATE POLICY EFFORTS
- Secured key improvements to the new Chronic Pain Management codes adopted by the Centers for Medicare & Medicaid Services (CMS) in the 2023 Physician Fee Schedule, following two years of collective advocacy that aided CMS in the development of the new codes.
- Issued a public comment to CDC regarding the draft version of the now-finalized Clinical Practice Guideline for Prescribing Opioids for Pain (2022). AACIPM, on behalf of 44 individual and organizational signatories, expressed support for a number of aspects of the proposed guideline, made a number of suggestions for improving the guideline, and outlined a number of ways that CDC could ensure a robust and effective dissemination effort related to the release of the updated guideline.
- Participated in the NCCIH Stakeholder Meeting for Research on Whole Person Health, emphasizing six key points in our testimony, including the need for agreement around quality standards and outcome measurements for CIH for pain and the need for collaboration on new funding opportunities to assess CIH approaches in the safety net, such as FQHCs.
- Disseminated timely federal policy changes, recommendations, and data to stakeholders, including the:
- CMS Behavioral Health Strategy, which outlines five major goals related to access to prevention and treatment services for substance use disorders, mental health services, crisis intervention and pain care, and enabling care that is well-coordinated and effectively integrated.
- AHRQ Systematic Reviews on Treatments for Chronic Pain, a comprehensive synthesis of the recent evidence from the peer-reviewed literature on the effectiveness and harms of noninvasive treatments for chronic noncancer pain. The reviews are presented in three reports: Opioid Treatments for Chronic Pain; Nonopioid Pharmacologic Treatments for Chronic Pain; and, Noninvasive Nonpharmacologic Treatment for Chronic Pain.
- VA/DoD’s Use of Opioids in the Management of Chronic Pain (2022), a joint guideline that is formatted as three algorithms and 20 evidence-based recommendations related to (a) determination of appropriateness for opioids for chronic pain, (b) initiation of treatment with opioids, and (c) maintaining, tapering, discontinuing, or switching from full agonist opioids.
- NAM Chronic Pain Journey Map, a visual illustration that identifies five key stages of the pain journey that have critical touchpoints with the health system, with each stage of the journey framed by lived experience perspectives, explaining what works well, common challenges, and identifies actions that specific health care stakeholders can take to improve the pain management process.
ADVOCACY, RESEARCH AND RESOURCES
- Developed and released an educational advocacy brief, Pediatric Pain: Promoting Access to Whole Person, Multimodal Pain Management for Children and Adolescents. The resource contains: extensive evidence-based tools and educational opportunities for health care providers; care options and support groups for patients and families; and, evidentiary support that can be used when discussing this issue with policymakers.
- Developed and released a CIPM Toolbox, a visual tool to illustrate and increase awareness of the various therapies that may be a part of whole person, multidisciplinary, multi-modal, evidence-informed, integrative pain management.
- Participated in the International Congress on Integrative Medicine and Health 2022, moderating a multi-stakeholder discussion about overcoming obstacles on the path to comprehensive integrative pain management.
- Updated our Resources for People with Pain, a repository of apps, books, websites, videos, blog posts, and support groups relevant to the advancement of comprehensive integrative pain management.
- Published a spotlight on newly elected representative Dr. Dave Nagel about pain, advocacy, and using one’s voice to spur change.
- Developed a presentation (to be done in January 2023) for Andrew Weil Alumni & Associates / fellowship graduates about Engaging in Advocacy to Advance Integrative Care on Local, State and Federal Levels.
STRENGTHEN PARTNERSHIPS / BUILD AWARENESS
- Aided in the development of Washington Health Alliance’s Tool for Low Back Pain, arranging and facilitating a group call with patient leaders to bring in the perspective of people with pain as WHA developed their tool.
- Developed The Role of Occupational Therapy in Comprehensive Integrative Pain Management in collaboration with the American Occupational Therapy Association, a resource intended to build awareness across stakeholders by providing context about occupational therapy as an important part of a quality interdisciplinary and integrative team.
- Promoted Pain & Self Care Awareness Month, collaborating with partner organizations to spread awareness and deepen connections and understanding among AACIPM’s diverse stakeholders.
- Discussed the Past, Present, and Future of PCORI with Dr. Christine Goertz and drew attention to PCORI’s calls for nominations to fill seats on its Board of Governors, Advisory Panels, and positions for Merit Reviewers and Peer Reviewers.
- Kept stakeholders apprised of relevant NIH HEAL Initiative funding opportunities as they became available through regular updates in our monthly newsletter, The Connector.
- Disseminated the updated Pain Management Guide from the National Football League Players Association, which covers a wide range of topics including: physical and restorative modalities, complementary and alternative therapies, medication, interventional therapies, regenerative therapies, pain and sleep, cannabis, psychotherapies, and more.
- Updated and improved our website to help stakeholders better find the information they need to advocate for improved pain management policies.
PROMOTE INNOVATION AND PROGRESS
- Developed and hosted Innovation in Advancing Equitable, Whole Person, Multimodal Pain Care, a webinar focused on advancements in multimodal pain care, with a focus on equity imbalance, from the perspective of public and private insurers, industry, healthcare providers, and people with pain.
- Announced the upcoming (January 25, 2023) webinar Realities, Research & Rethinking Person-Centered, Integrative Pain Management, which will bring together perspectives from people with pain, research, clinical practice and payers to discuss innovation and progress in their field and how to keep people with pain at the center of this care.
- Curated the Repository of Clinical Practice Examples: Innovation and Progress to better share with stakeholders current clinical practice examples that advance equitable, whole person centered, multi-modal pain management.
- Collaborated with the American Medical Association to highlight Inner Atlas, a unique method of facilitating whole person, multimodal pain care.
ADDRESS EQUITY ISSUES
- Provided NCCIH with a list of determinants for whole person health to aid the agency is identifying a set of just twenty factors that influence health, either positively or negatively, and that encompass the full continuum of the human experience (biological, behavioral, social, and environmental).
- Highlighted new data from Optum Labs that shows vast disparities in pain care across geographically dissimilar zip codes in the United States.
- Participated in the Total Force Fitness (TFF) – Whole Health (WH) Summit, a two-day summit held jointly by the Department of Defense (DoD) and Department of Veterans Affairs (VA), which explored how DoD’s TFF and VA’s WH programs may be optimally linked for the benefit of transitioning service members.
- Ongoing collaboration about equity issues with National Pain Advocacy Center, Integrative Medicine for the Underserved and other groups, resulting in activities such as scholarships for education for health professionals caring for people who are underserved.