CIPM Toolbox
Comprehensive Integrative Pain Management (CIPM)
What is CIPM?
Comprehensive integrative pain management (CIPM) includes biomedical, psychosocial, complementary & integrative health, and spiritual care. It is person-centered and focuses on maximizing function and wellness. Care plans are developed through a shared decision-making model that reflects the available evidence regarding optimal clinical practice and the person’s goals and values.
This definition was crafted with input from over 50 national organizations representing people with pain, health care providers, public and private payers, researchers, advocates and policymakers—but what does it really mean?
First and foremost, the person living with pain is at the center of a CIPM care plan.
Policies that promote CIPM encourage a shared decision-making model that reflects the available evidence regarding optimal clinical practice and the person’s goals and values. The aim is to provide the right care at the right time – tailoring a treatment plan that will best support them in achieving those goals. This includes asking “What matters to you?” and not “What’s the matter with you?”
Once the individual’s goals have been established, a CIPM treatment plan can be developed.
Each person’s situation is unique and social determinants of health need to be considered when integrating and developing a treatment plan (e.g., diagnosis, co-morbidities, support systems, goals and responsibilities, resource availability, etc.) It is not one size fits all.
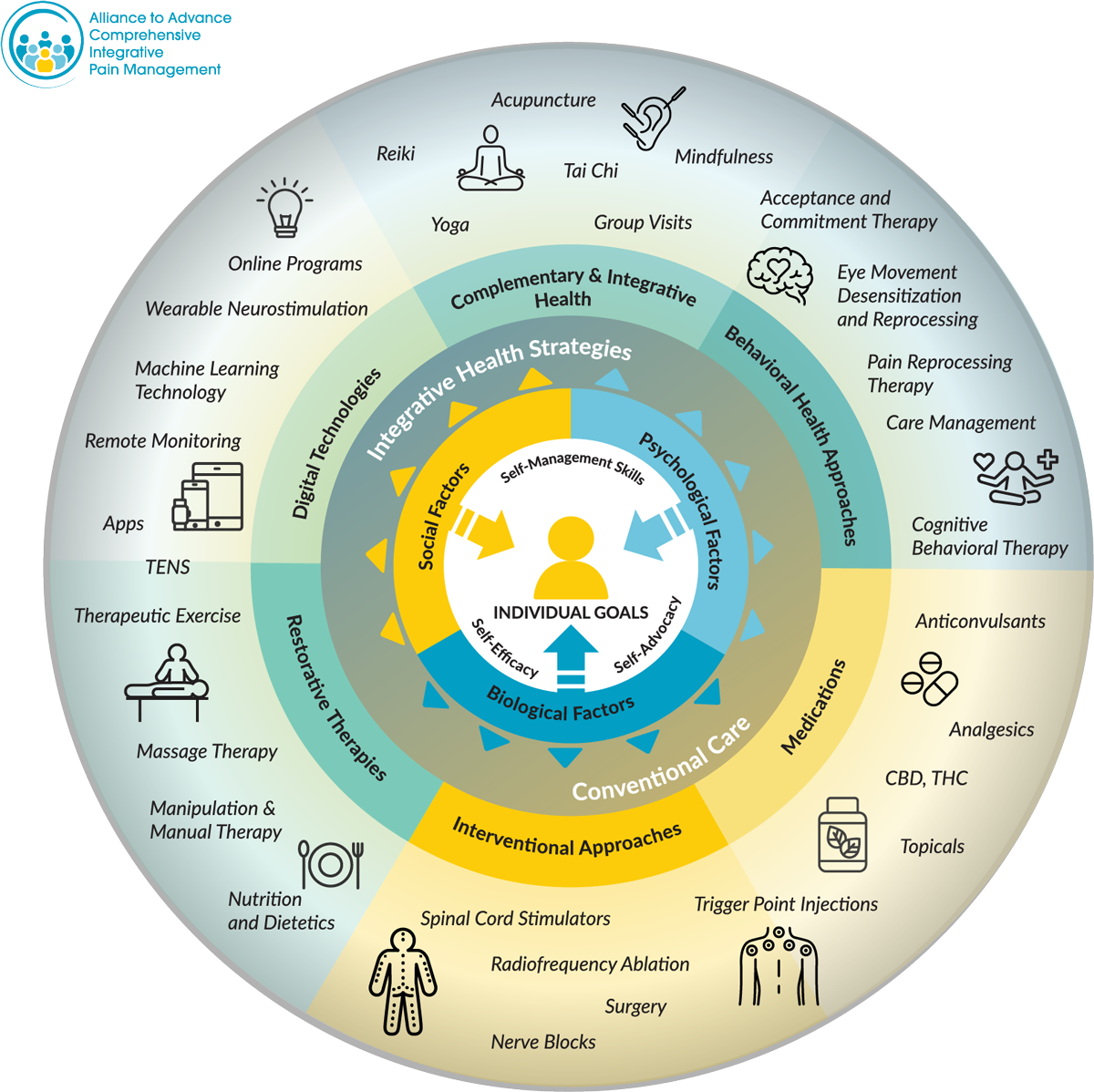
The “CIPM Toolbox” illustrates the range of pain care therapies.
This is not an exhaustive list of available pain management therapies, and not all therapies will be appropriate for all individuals. A primary care provider, integrative care team, or other health care provider will help each person with pain to determine which treatments, referrals, and self-care options will make up an optimal care plan.
#RightCareAtTheRightTime #WhatMattersToYou
Citation: Comprehensive Integrative Pain Management Toolbox. Alliance to Advance Comprehensive Integrative Pain Management. August 2022. https://painmanagementalliance.org/what-is-cipm/
AACIPM offers this visual tool to illustrate and increase awareness of the various therapies that may be a part of whole person, multidisciplinary, multi-modal, evidence-informed, integrative pain management.
This does not represent an exhaustive list of interventions, and not all interventions will be covered, covered without limits and/or without patient out-of-pocket cost.”
Most services must be provided by a licensed or credentialed health care provider or community-based service provider.
Sign up to receive our updates